Causes of IVF failures
IVF cycle includes several phases, and each of them should be successfully accomplished before passing to the next step:
- growth and development of at least one follicle should start
- follicles should get matured
- no premature ovulation should start before the follicle puncture
- oocytes should be successfully extracted from follicles during the puncture
- spermatozoa should fertilize at least one oocyte
- fertilized oocyte should start partitioning and developing
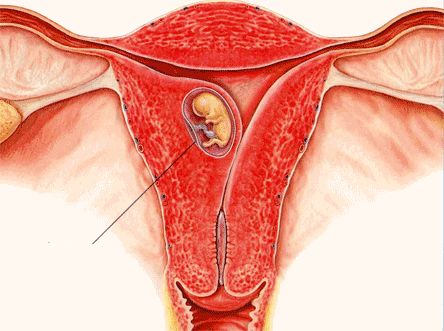
- embryo should be implanted in the uterus
In this chain the implantation is still a mystery for scientists – why doesn’t each embryo become a child?
Using modern technologies we succeed in generation of embryos in the laboratory, but we still can't control the implantation process. We don’t know which embryo will become a child and this brings disappointment to both doctor and patient.
The hatched blastocyst should then be implanted in the uterine endometrium within a short period of time called an implantation space of time. The three main implantation phases are opposition, adhesion and invasion. The opposition or ebryo orientation in the uterine cavity starts at the moment when the uterine cavity is maximally reduced because of absorption of a fluid in it.
Blastocyst adhesion is a chain of biochemical reactions resulting in blastocyst attachment to the endometrium. Many molecules, such as cytokines, growth factor and integrins play an important role in this complicated process when the blastocyst and maternal endometrium enter into a thin “dialogue”.
Invasion is the most controlled process allowing embryonic trophoblast (blastocyst cells which afterwards will become placenta cells) to deeply penetrate into the decidual maternal tissue (endometrium cells which will as a result form the maternal part of the placenta) and penetrated into the endometrium blood flow. This takes place due to generation of special chemical agents called proteinase.
Immune mechanisms, ensuring dialogue between maternal tissues and embryo, are very important for the successful blastocyst implantation. Activated cells of the decidual tissue and trophoblast cells generate a big number of immunologically active agents provoking necessary immune reactions.
It’s still a mystery how implantation is regulated and takes place, but it’s worth mentioning that people interestingly have low implantation efficiency. Absolutely healthy married couple has only 20-25% probability for conception in each menstrual cycle. The responsibility for such low efficiency is borne both by the embryo and abnormalities in embryo-endometrium dialogue. Today we know that one of the major reasons of failed implantations are embryo's genetic pathologies. Fundamental researches in the sphere of implantation are quite interesting, as the implantation itself is the main factor limiting the ART efficiency. However we need to study a lot of things before we can truly control this process.
Analysis of failed IVF cycle
 If you don’t get pregnant after the first IVF attempt, of course, you’ll be upset and disappointed. However, you should remember that this is not the end – that’s only the beginning. After the failed IVF attempt you’ll meet the doctor and will analyze all possible conclusions. When analyzing the failed IVF attempt the doctor will pay special attention to the quality of embryos, as well as other important points:
If you don’t get pregnant after the first IVF attempt, of course, you’ll be upset and disappointed. However, you should remember that this is not the end – that’s only the beginning. After the failed IVF attempt you’ll meet the doctor and will analyze all possible conclusions. When analyzing the failed IVF attempt the doctor will pay special attention to the quality of embryos, as well as other important points:
- Was the organism prepared for the pregnancy? Of course, the fact of availability of general gynecological diseases doesn’t always influence on the pregnancy, but from the other side the reduction of conception capacities shouldn’t be excluded in case of such diseases. Therefore the organism should be prepared for conception and IVF in the conditions of lack of any chronic disease.
- Was the ovary response to the stimulation good enough?
- Did the fertilization take place?
- Were high quality embryos generated, did they normally get developed in laboratory conditions?
- Was the thickness and construction of the endometrium optimal at the moment of transfer?
- Were any abnormalities in the endometrium development detected during the IVF program?
- Did the implantation take place defined by the blood test to check the level of HCG hormone two weeks after the embryo transfer?
- Why hasn’t the pregnancy started? (although there is no answer to this question)
- Is it necessary to conduct any additional examination before the next IVF cycle?
- Is it necessary to undergo any treatment before the next IVF cycle?
- Can the same regimen be repeated or does it need some changes before the next attempt?
- When can the IVF recycle start?
IVF recycle
The most doctors recommend to wait for at least a month before the start of the next treatment cycle. Although the IVF recycle can be conducted in the next month the most of patients need a break to muster up their strength and restore emotional balance. As a rule we recommend a three month break before the IVF recycle.
Depending on the results of the previous cycle the doctor may need to change the treatment regimen. E.g. if the ovary response to the stimulation was insufficient, the doctor may increase the dose of medications for the stimulation of superovulation or to change the stimulation protocol. If the fertilization didn’t take place, you may need ICSI. If the quality of oocytes was poor the doctor may recommend using donor oocytes. However if the results of the previous cycle were satisfactory the doctor may recommend to repeat the same treatment regimen.
It’s interesting that couples undergoing IVF recycle are calmer and control the situation more competently. Probably this is conditioned with the fact that they’re aware of necessary medical procedures and are well prepared.

















































